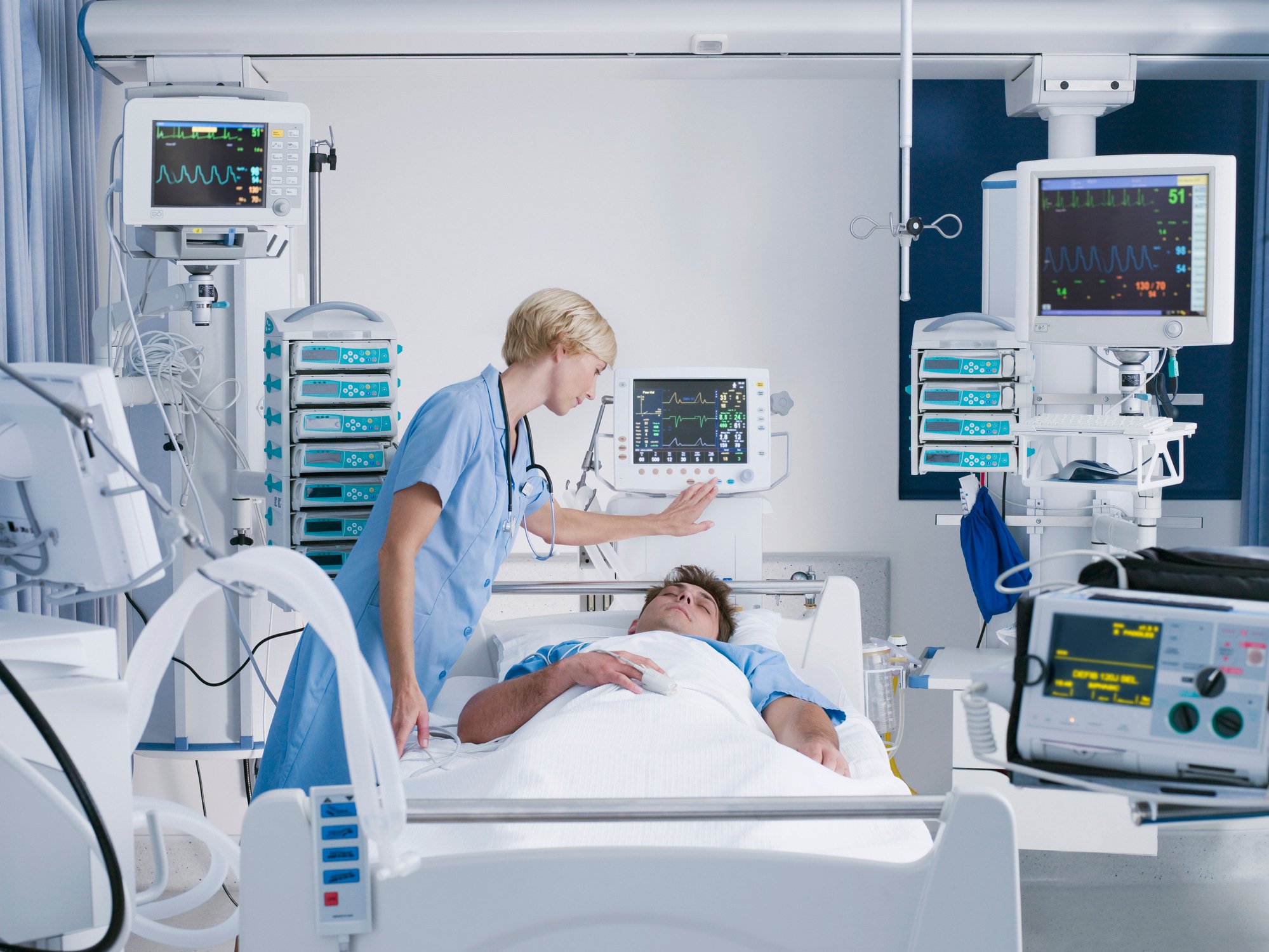
Recognizing Hemodynamic Changes in Your Patient
A critically ill patient represents the most unpredictable patient. Knowing how to recognize changes that require early intervention increases your value at the bedside. Using this knowledge to anticipate what medical treatments will be utilized helps you prepare and care for this patient.
Hemodynamic monitoring is a standard of care in most intensive care units (ICU). Many patients in the ICU will have an arterial line to monitor blood pressure and allow the nurse and respiratory therapist to draw arterial blood gases and laboratory samples without additional venipunctures. Additionally, to assist with fluid resuscitation, blood product administration, parenteral nutrition, and medication administration, central venous lines are placed (Villa, Ricci, & Romagnoli, 2019).
In some patients, these two lines are not enough to divulge what may be occurring within the cardiac system. At this time, a practitioner may decide to place a pulmonary artery catheter. This catheter, while measuring the pressure of the right ventricle as a CVP line does, also measures the left heart pressures, and allows cardiac output measurement, mixed venous oxygen saturation monitoring, and specimen sampling (Bonsall, 2016).
Care and maintenance of these lines fall to the critical care nurse. Ensuring the pressure readings are accurate by leveling, zeroing, and square testing each hemodynamic line each shift, recognizing normal and abnormal waveforms, and recognizing normal and abnormal pressure readings will help the nurse and practitioner manage the patient in a timely manner.
One critical aspect of invasive hemodynamic monitoring is the ability to measure cardiac output, the amount of blood pumped into the aorta each minute, and cardiac index, a patient’s cardiac output based on their body surface area (BSA). Additionally, a solid understanding of preload, afterload, systemic vascular resistance, stroke volume, and pulmonary vascular resistance is necessary to understand the impact of each measurement.
If you need assistance, the RN.com course, Principles of Invasive Hemodynamics was written to help not only novice ICU nurses but also experienced nurses sharpen their hemodynamic monitoring skills. This module contains explanations of hemodynamic concepts so essential to patient care.
Knowing how hemodynamic monitoring devices can improve your assessment skills is something every ICU nurse should learn and practice.
References
Bonsall, L. (2016). Cardiac output and cardiac index – what’s the difference. Villa, G., Ricci, Z., & Romagnoli, S. (2019). Chapter 4-Hemodynamic support in the critically ill patient in Critical Care Nephrology (3rd Ed., pp. 21-25, e2). Philadelphia, PA, Elsevier.




